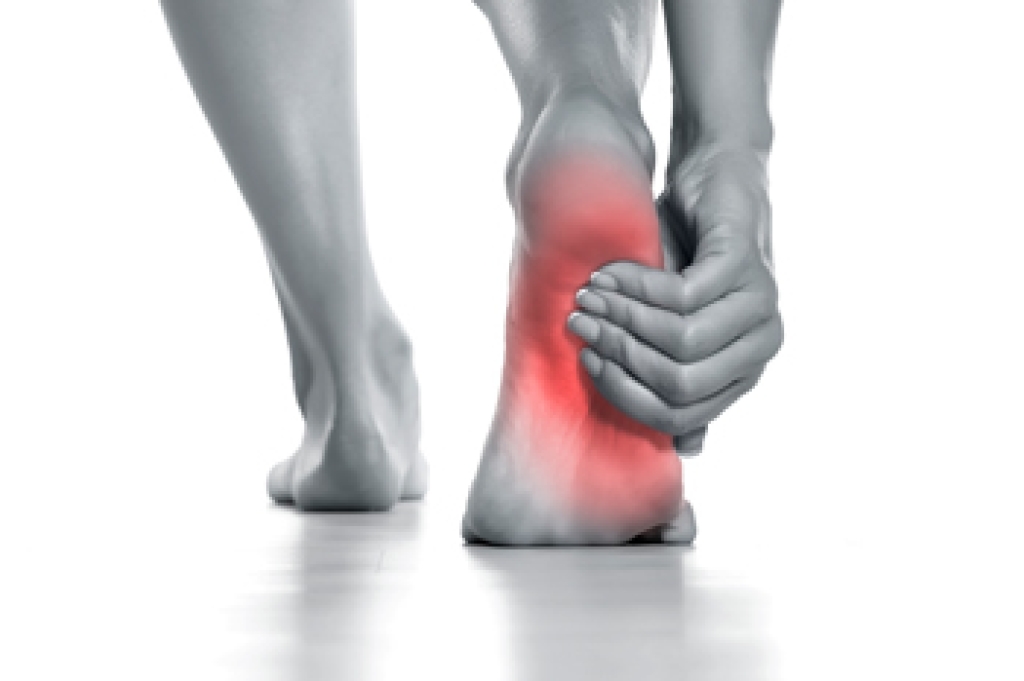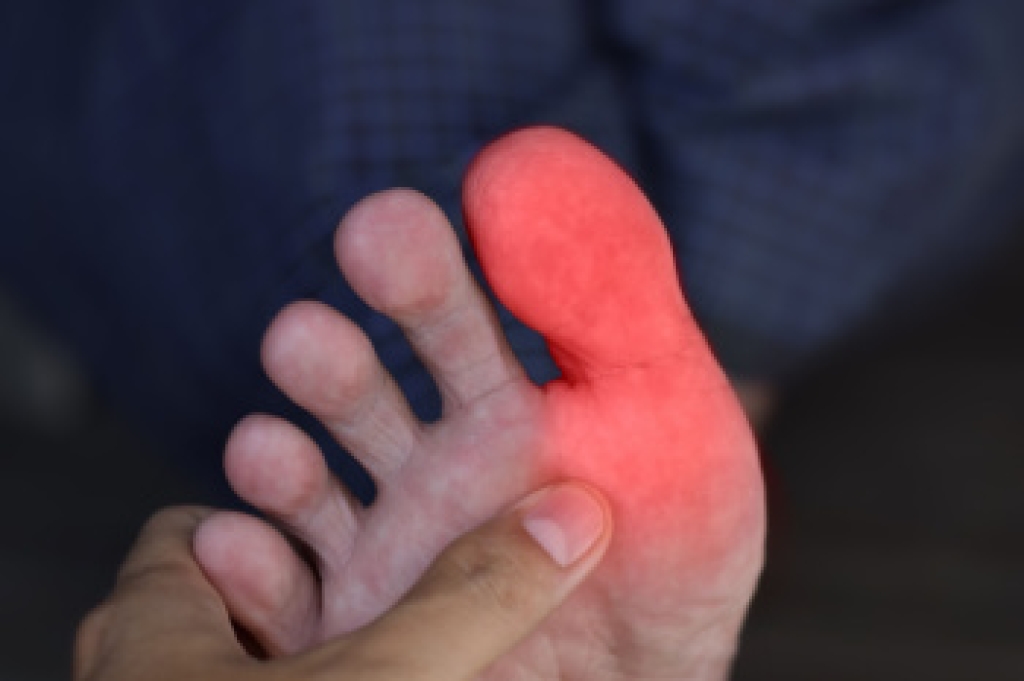
Sharp pain in the big toe that develop suddenly may point to several underlying conditions. An ingrown toenail occurs when the nail grows into the surrounding skin, causing redness, swelling, and tenderness. Gout is a form of arthritis that results from uric acid buildup, often leading to intense pain, warmth, and swelling in the big toe joint. Additionally, a broken toe can happen from direct impact or trauma and may cause bruising, stiffness, and difficulty walking. Risk factors include improper nail trimming, certain medical conditions, injury, and footwear that places pressure on the toes. Each cause may affect the toe differently, but ongoing pain should not be ignored. A podiatrist can evaluate the source, provide accurate diagnosis, and guide proper treatment. If you have discomfort in your big toe, it is suggested that you visit a podiatrist who can offer appropriate relief and treatment solutions.
Toe pain can disrupt your daily activities. If you have any concerns, contact one of our podiatrists of The Foot Specialists. Our doctors can provide the care you need to keep you pain-free and on your feet.
What Causes Toe Pain?
Most severe toe pain is caused due to a sports injury, trauma from dropping something heavy on the toe, or bumping into something rigid. Other problems can develop over time for various reasons.
Toe pain can be caused by one or more ailments. The most common include:
- Trauma
- Sports injury
- Wearing shoes that are too tight
- Arthritis
- Gout
- Corns and calluses
- Hammertoe
- Bunions
- Blisters
- Ingrown toenails
- Sprains
- Fractures (broken bones)
- Dislocations
When to See a Podiatrist
- Severe pain
- Persistent pain that lasts more than a week
- Signs of infection
- Continued swelling
- Pain that prevents walking
Diagnosis
In many cases the cause of toe pain is obvious, but in others, a podiatrist may want to use more advanced methods to determine the problem. These can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatments for toe pain and injuries vary and may include shoe inserts, padding, taping, medicines, injections, and in some cases, surgery. If you believe that you have broken a toe, please see a podiatrist as soon as possible.
If you have any questions please contact our offices located in Waltham and Milford, MA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.